Breast Augmentation
One generally accepted standard for being considered beautiful, feminine, and always well put together is having a fit, proportional physique. Maintaining that look can be difficult when aging, childbearing, or simply Mother Nature causes you to feel dissatisfied with your breast size. With breast augmentation at our Grapevine practice, you can have your ideal breasts and the self-confidence that comes with them.
Communities We Serve
Women throughout Texas seek out Dr. Bogdan and Dr. Cason for their artistry, surgical skill, and compassionate bedside manner. We regularly see patients from the following communities, which are a short drive from our Grapevine plastic surgery practice:
- Fort Worth
- Frisco
- Plano
- The larger Dallas-Fort Worth (DFW) metro region
Breast Augmentation
Before & After Photos
This gallery contains images intended for adult audiences.
VIEW PHOTOS
How Much Does Breast Augmentation Cost in Fort Worth?
The cost of breast augmentation depends on multiple factors, including your choice of breast implants, the complexity of the surgery, and whether it will be combined with other procedures such as a breast lift or tummy tuck. Although cost is a necessary consideration, choosing a well-trained plastic surgeon with extensive experience performing breast enhancement surgery is important. You will receive a personalized price quote at the end of your consultation.
Performing Breast Augmentation
Breast augmentation is a very personal decision, and your breast augmentation procedure will also be highly personalized. In order for your procedure to be specifically tailored to your unique needs and desires, many subsequent decisions must be addressed. One of the most common concerns patients want to address is, “What will I look like with a certain size implant?” Although before-and-after-photo galleries help assess a surgeon’s skill and aesthetics, it may be difficult to find a patient that exactly matches your body type and desires. To address this issue, in our Grapevine plastic surgery office, our physicians utilize 3D imaging to simulate operative outcomes on your own body.
Choosing the Right Breast Implants For You
Both saline and silicone implants are approved for use in primary breast augmentation. As with any surgical operation, you must weigh the pros and cons of specific choices and decide which option is best for you. Dr. Michael Bogdan and Dr. Roger Cason have experience with both saline and silicone implants. At your consultation, they will take the necessary time to go over your options and guide you toward getting the results you want.
Saline Breast Implants
Saline-filled implants were the only option for women seeking breast augmentation between 1992 and 2006. That changed when silicone-filled breast implants came back on the market. Saline implants filled with a medical-grade saltwater solution pose no health risks. If they rupture or leak, the saline is harmlessly absorbed by the body and eliminated. Due to lower manufacturing costs, traditional saline implants cost less than silicone gel-filled implants. And since they are filled during the surgery, our surgeons have some ability to “fine tune” the size of each implant for your procedure.
Most women report the biggest drawback to traditional saline-filled implants is that they tend to look and feel less natural than silicone gel implants. Saline implants, for example, may show wrinkles or ripples, particularly for women with little existing breast tissue or when the implants are placed above the pectoral muscle. Also, if one of these implants leaks or ruptures, there is an immediate and conspicuous loss of volume, which makes revision surgery a more urgent concern.
Silicone Gel Implants
Technological advances have led to the development of cohesive silicone gel implants that most patients and surgeons believe look and feel more like natural breasts than traditional saline implants. The gel that fills the implants is much less likely to leak if punctured, torn, or cut. To ensure ongoing safety, the FDA continues to monitor silicone implants as part of a post-approval study.
Like women worldwide, the vast majority of women having breast augmentation in Plano, Frisco, and throughout the Dallas-Fort Worth area choose silicone gel implants. They rarely ripple or wrinkle and do not slosh like traditional saline implants sometimes do, which is one of the reasons why many women are trading out older saline implants for silicone gel. Our practice uses gel implants from the top manufacturers: Mentor, Allergan, and Sientra.
Implant Comparison
Here are some points to consider in choosing the right breast implants:
Similarities
- Both implants add volume to the breast
- Both are available in several shapes, sizes, and textures
- Both implants have a silicone elastomer shell. Since the shell is flexible, it has the possibility of developing fatigue cracks and leaking during the life of the implant
- Surgical risks (such as bleeding, infection, scar, deflation, capsular contracture, etc.) are present with both implants
Differences
- Saline implants generally cost less than silicone implants
- Silicone implants are thought to feel more like breast tissue
- Silicone implants have less visible rippling than saline implants
- Implant tears are easier to identify with saline implants
- FDA restricts the use of silicone implants for women who are 22 or older; saline implants are approved for women who are at least 18 years old
- FDA recommends MRIs to check for wall ruptures in silicone-gel filled implants starting 5 to 6 years after surgery
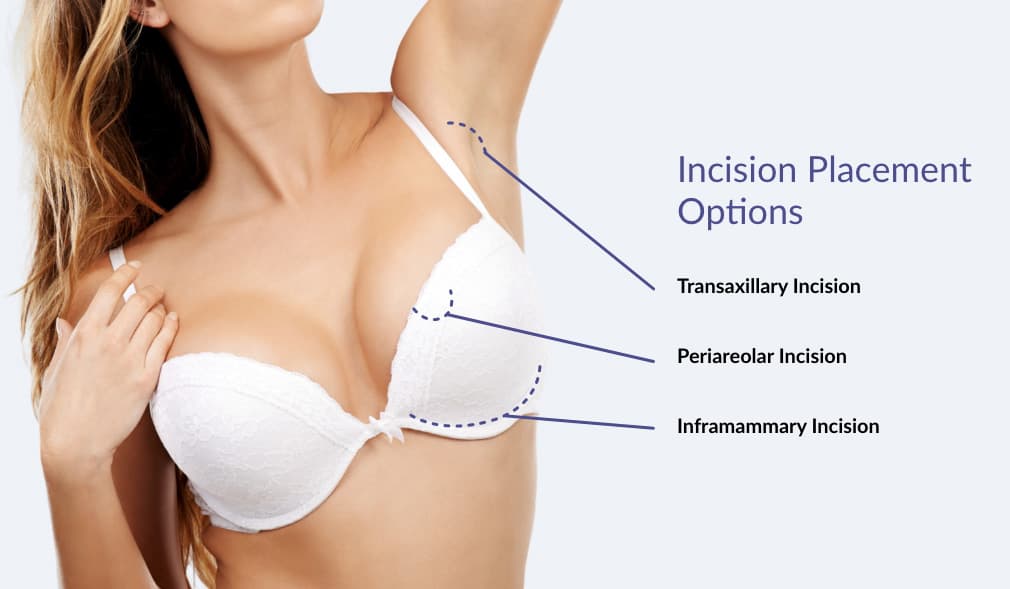
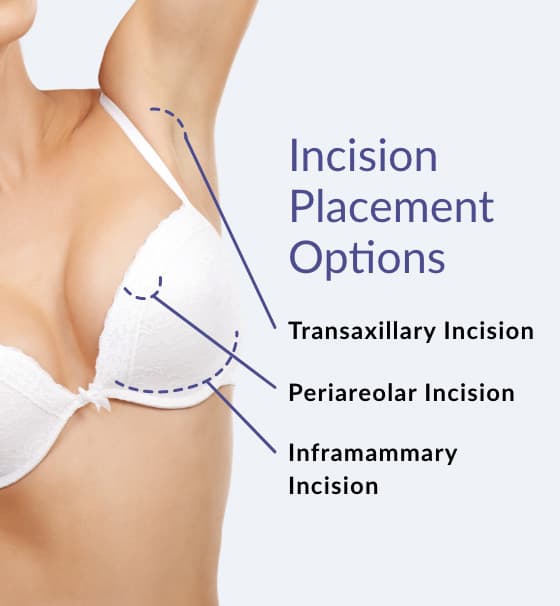
Your Incision Placement Options
Another decision to be made is where to place the incisions. There are many factors to be weighed when considering incision types, such as the degree of enlargement desired, your existing breast anatomy, your personal preference, and your breast implant type. Dr. Bogdan and Dr. Cason strive to minimize scarring and will work with you to determine which incision method is right for your needs.
Your Breast Implant Placement Options
After choosing the incision site, you and your physician will select the appropriate implant placement. Breast implants can be placed either beneath the pectoral muscle (submuscular) or over the pectoral muscle (subglandular). Where to place the implant depends on various factors, including the degree of augmentation desired, the type of implant selected, and your particular anatomy.
- Submuscular placement is the more commonly used of the two methods for women undergoing breast enlargement in DFW. Both saline and silicone gel implants are regularly inserted using this method, which tends to produce a more natural appearance for most body types. In addition, recent studies suggest that submuscular placement decreases the risk of capsular contracture, a complication in which excess scar tissue tightens around the implants. Due to the incision of the muscle tissue, this method may result in a more extended recovery period with slightly more discomfort.
- The subglandular method places the implant behind the breast tissue but above the pectoral muscle. This method results in a more comfortable recovery but may be more likely to interfere with mammograms. However, less tissue over the implant means the implants are more visible and may look less natural. Women with thin skin or very small breasts are not good candidates for this option.
Get to know our board-certified Dallas-Fort Worth plastic surgeons Dr. Michael A. Bogdan and Dr. Roger W. Cason. With decades of combined experience, they received their education and fellowship training at some of the most prestigious institutions in the country, including Stanford, Duke, and New York University.
Can Breast Augmentation Surgery Be Combined With Other Procedures?
Yes. Many women have multiple areas they’d like to improve, so we often combine breast augmentation with other procedures, including:
Combination breast and body procedures are often called Mommy Makeovers because they are popular with women after pregnancy and breastfeeding.
Breast Augmentation vs. Breast Lift
For some women, it is perfectly obvious whether breast augmentation or a breast lift will achieve the desired result, but for others, the situation is not so clear. If your breasts sag (“ptosis”)—whether from weight fluctuations, breastfeeding, aging, or genetics—breast implants alone may not give you the results you want. You may need to combine breast augmentation with breast lift surgery to create fuller and perkier breasts.
How Long Does It Take To Recover From a Breast Augmentation?
Recovery rates vary between breast augmentation patients, but they generally follow this timeline:
- Stop pain medication: 2 to 3 days post-op
- Return to work or school: 1 week
- Incisions healed: 1 to 2 weeks
- Resume light exercise: 2 weeks
- Resume upper-body exercise: 3 weeks
- Swelling subsides: 6 to 8 weeks
- Breasts soften/implants drop: 6 to 8 weeks
- Achieve final results: 3 months
Deciding to have breast augmentation is the beginning of a journey to a new and improved you. Along the way, you will face numerous choices, and Dr. Bogdan and Dr. Cason will help you carefully weigh your options. Their extensive training and experience performing breast augmentation help them to customize each procedure to the needs of each patient. It’s essential to follow your post-op instructions closely to optimize healing and results.
After breast augmentation, we may have you perform breast implant exercises to maintain soft and natural-feeling breasts. Please review the Breast Implant Exercises page so you will have an understanding of the exercises before your consultation.
Breast Augmentation FAQ
How long is the surgery?
With the inframammary fold approach, breast augmentation surgery takes 30 to 60 minutes. The time variations arise due to differences in anatomy. The transaxillary approach is technically more demanding, taking up to 30 minutes longer.
What type of anesthesia is used?
Dr. Bogdan and Dr. Cason recommend a general anesthetic for breast augmentation surgery. While it is true that breast augmentation can be performed with a different anesthetic, it is not ideal. General anesthesia allows the surgeon to perform more extensive and intricate dissection than possible with sedation surgery, making it safer for the patient. When you’re under general anesthesia, you have an anesthesiologist fully concentrating only on your comfort and vital functions. At the same time, the surgeon is free to fully focus on obtaining the desired surgical result.
How much time off work and exercise will I need?
About 80% of patients should be able to return to desk work 2 days after surgery. Recovery after breast augmentation surgery depends a lot on how much you expect from your body. As with any surgery, there is always a risk of bleeding after the operation, so we recommend that you abstain from any activity that would raise your blood pressure or heart rate for 2 weeks after surgery. This includes exercising, strenuous activities, or lifting more than 15 lbs.
How painful is breast augmentation surgery?
The amount of discomfort an individual patient experiences depends on several factors, including overall pain tolerance, the size of the implant chosen (larger implants create more stretch and thus hurt more), and how easily the breast accepts the implant. In general, most women feel noticeable discomfort requiring medications for the first 2 days after surgery. Then they will have tolerable discomfort during the daytime, reserving pain medications for nighttime use to help with sleep.
How soon will I be able to return to a full-body workout?
Our physicians recommend avoiding all exercise for the first 2 weeks after surgery to reduce the chance of post-operative bleeding. You can walk as far as you like—but at a sightseeing pace rather than an aerobic pace. After 2 weeks, you can start lower body exercise and resume upper body exercise at 3 weeks. Regular athletic women will feel back to normal about 6 to 8 weeks after surgery. Extreme athletes who demand more from their pectoral muscles will take longer to recover (3 to 6 months).
How will surgery affect nipple sensation?
It is very typical to have an altered nipple sensation for some time after breast augmentation. The implant adds volume to the breast, stretching the skin and the nerves that run through the skin. The nerves tend to fire off more easily or sometimes don’t transmit signals well after surgery. For these reasons, the nipple may become temporarily hypersensitive or less sensitive after surgery, typically lasting 1 or 2 months. During this time, slight contact on the nipple (such as clothing brushing lightly across it) may make it feel like it is on fire. Silicone nipple shields can make this more tolerable. Aside from the nerves being stretched, there is a possibility that the nerves important for nipple sensation may pass right through where the implant needs to be. If this is the case, the nipple sensation may be permanently lost, but this does not happen often.
How soon can I have breast implants after childbirth?
The timing for breast augmentation depends more on when you stop breastfeeding than when you give birth. It is reasonable to consider augmentation somewhere between 3 to 6 months after finishing breastfeeding. When you stop breastfeeding, it will take time for your breasts to stop involuting (shrinking). You want to be sure that your breasts have stopped shrinking before considering augmentation; otherwise, your breasts will not be as full as desired after surgery.
Do I need to have a mammogram before surgery?
Dr. Bogdan and Dr. Cason recommend a screening mammogram within the last year for all women over 40 (or 30 for those with a strong family history of breast cancer). Breast enhancement surgery significantly changes the breast in several ways, elevating the breast tissue off the chest and reducing the amount of breast tissue that can be seen in mammograms.
How will smoking affect my surgery and recovery?
We recommend stopping smoking and nicotine products for 3 weeks before and after surgery for breast augmentation. Everyone knows smoking is bad for your health and increases the risk of getting cancer. From a cosmetic surgery standpoint, smoking increases both short-term and long-term risks. Nicotine use has a vasoconstrictive effect, slowing blood flow. Peripheral tissues like the skin really see this effect. Chronic smoking accelerates skin aging by reducing the ability of the skin to heal from the constant damaging forces of everyday life (such as sun exposure). This means skin wrinkles faster in smokers than non-smokers and will also stretch out more quickly as youthful, elastic skin properties are lost. For implants, this means “perky” breasts will drop faster, and the chance of implants “bottoming out” is higher. In the short term, smoking around the time of the operation increases all surgical risks due to reduced blood flow and delayed healing. Scars will tend to be wider and more visible, with higher infection rates.
What is capsular contracture, and how can I prevent it?
Capsular contracture is the hardening of the breasts caused by the aggressive shrinking of the scar capsule around the breast implant. Any time an implant is placed in the body, it will be encased in a layer of scar tissue. For most types of implants (such as chin implants lying on the jaw bone), it does not matter if the scar capsule shrinks tightly. Breast implants are a different matter—in this setting, we do not want the scar capsule to shrink. If the scar capsule around the implant is soft and wider than the implant, it won’t be noticed at all. If the scar is thick, aggressive, and shrinks tightly around the implant, it will feel like a rock in the breast.
There are several theories as to why a patient might form this type of aggressive scar, the two most relevant being a genetic predisposition to aggressive scars or an irritant such as a low-grade infection hiding on the implant wall. There is no way to test to see if you have a genetic predisposition for aggressive scarring–and luckily, this does not happen often. We can take steps to reduce other possible causes of capsular contracture, including using current-generation implants and antibiotics. With smooth implants, Dr. Bogdan and Dr. Cason recommend performing displacement exercises to decrease the chance of capsular contracture.
What are BII and BIA-ALCL?
Patients who are considering breast enhancement or currently have implants should be aware BII and BIA-ALCL, both of which are receiving media attention. Knowledge of the current scientific understanding of implants and associated risks should help alleviate stress caused by social media and news coverage.
I’m under 18 and am very self-conscious about my breasts. Can I get implants?
If breast augmentation is performed for reconstructive reasons (such as significant breast asymmetry), it can be performed for people under 18 with parental consent. If augmentation is desired for strictly cosmetic enhancement, the FDA approves saline implants for women 18 and older and silicone for ages 22 and up.
Will a specific size implant give me the desired cup size I want?
Choosing the right size implant is related more to your breast dimensions and skin elasticity than cup size. Bra manufacturers are not uniform in their sizing, so a better way to predict satisfaction with your results is to look at before-and-after photos of similarly built women. Dr. Bogdan and Dr. Cason both use sophisticated Vectra XT 3D imaging technology to predict surgical outcomes so that you can see how your body will look with different-sized implants.
Will exercising the pectoral muscles affect the results of implant position?
With sub-pectoral placement of the implants, the muscles can affect implant position. The implants are partially covered by the muscle, so muscle action will attempt to “squeeze” the implant out from underneath, translating to the implant moving down and to the side. Smooth implants are mobile and potentially could “drift” in this direction due to muscle action. To prevent this from happening, our physicians recommend that patients perform upward breast implant displacement exercises to counteract this muscle action.
Do you recommend placing the implant under the muscle?
Both saline and silicone implants have the risk of being “seen” through the skin—either in the form of ripples on the implant surface or seeing the edge of the implant. The chance of this happening is related to how much coverage you have over the implant. Women who are very thin and athletic are more at risk for visible ripples than more fully proportioned women. Sub-muscular placement creates a more natural appearance in the short and long term and improves breast cancer surveillance with mammograms (compared to above the muscle placement). Additional data suggests implants placed below the muscle may have lower capsular contracture rates.
I have lost quite a bit of weight, and my breasts are deflated. Will implants fix them?
It depends on how deflated your breasts are and the look you hope to achieve. For some women, augmentation alone will deliver the desired appearance. For women who have a significant amount of droop and want perky breasts that are not overly large, a breast lift or a breast lift followed by breast augmentation is often needed to attain the desired result.
Will a specific size implant give me the desired cup size I want?
Choosing the right size implant is related more to your breast dimensions and skin elasticity than cup size. Bra manufacturers are not uniform in their sizing, so a better way to predict satisfaction with your results is to look at before-and-after photos of similarly built women. Dr. Bogdan and Dr. Cason both use sophisticated Vectra XT 3D imaging technology to predict surgical outcomes so that you can see how your body will look with different-sized implants.
Your Next Step
Choosing to have breast augmentation surgery and selecting the right breast implants is not a one-size-fits-all process. There are numerous considerations, such as your particular anatomy, lifestyle, and the look and feel you hope to achieve. Our fellowship-trained DFW plastic surgeons, Dr. Bogdan and Dr. Cason, have the experience and knowledge to help you explore your personal goals, develop a treatment plan, and choose the most appropriate implant for you.
Please request a consultation with one of our surgeons using the online form, or call our office at
(817) 442-1236 to schedule an appointment. We will be sure to answer all your questions so you feel confident with your choices throughout your aesthetic journey.
Breast Augmentation Related Blog Posts